What is Diabetic Retinopathy?
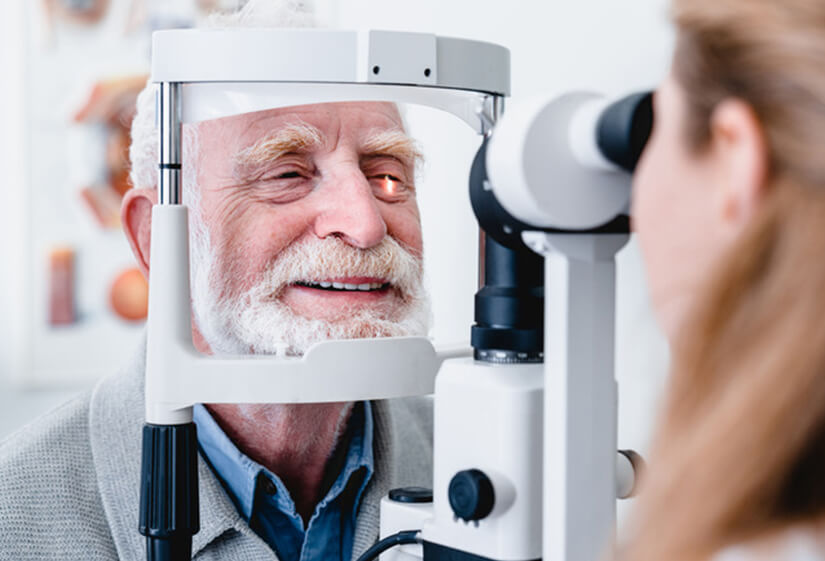
Diabetic retinopathy is a serious eye condition that affects people with diabetes. It occurs when high blood sugar levels, a common symptom of diabetes, damage the blood vessels in the retina. People with type 1 and type 2 diabetes are both at risk, although those with type 1 diabetes are more likely to develop severe types of retinopathy and require diabetic retinopathy treatment early in life.
The retina, positioned in the back of the eye, is a light-sensitive tissue that transmits nerve signals to the brain when exposed to light. The brain then processes these signals to produce visual impressions. When blood vessels inside the retina are damaged, they can become clogged, resulting in decreased blood flow to the retina. This reduced blood flow might cause the formation of new, abnormal blood vessels. These newly created vessels have the potential to leak and cause scar tissue to develop, resulting in decreased vision.
Diabetic retinopathy is a non-reversible condition. As the duration of diabetes increases, the likelihood of developing diabetic retinopathy also rises.
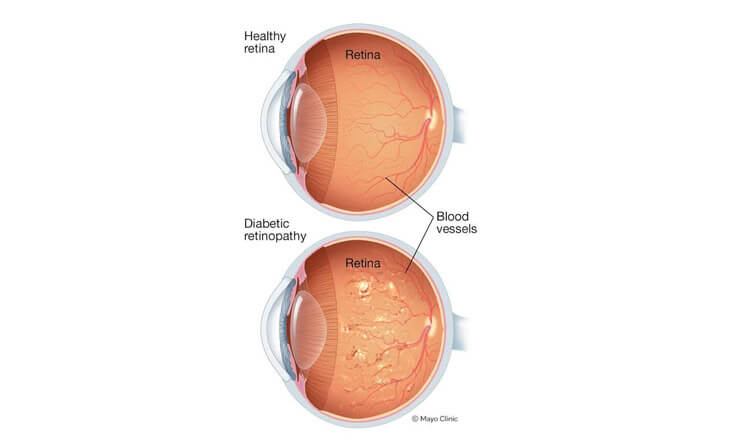
There are two types of diabetic retinopathy:
Nonproliferative Diabetes-Related Retinopathy (NPDR): During the initial stage, the blood vessels in the retina weaken and develop small bulges, known as microaneurysms. These weak blood vessels can leak blood and fluid into the retina, causing swelling and macular edema. This leakage and swelling could potentially affect vision. This stage might not always have noticeable symptoms. Only when the central part or the macula is involved, you will feel visual issues.
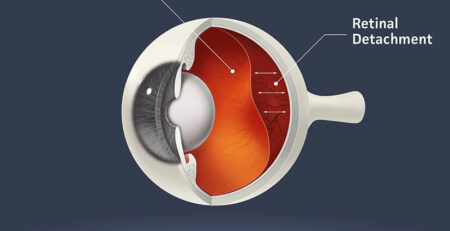
Proliferative Diabetic Retinopathy (PDR): As the disease progresses, new, abnormal blood vessels start growing on the retina’s surface. These new blood vessels are fragile and prone to bleeding, which can cause severe vision problems and even blindness if left untreated. Scar tissue may also form, leading to retinal detachment and further vision loss. Slight bleeding within the eye can lead to visual symptoms, such as dark spots and lines. In more severe cases of bleeding, significant vision loss can occur, which might cause blindness.
Diabetes duration, especially over 10 years, poor blood sugar management, high blood pressure, and high cholesterol are all risk factors for diabetic retinopathy.
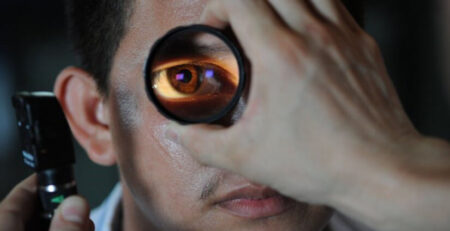
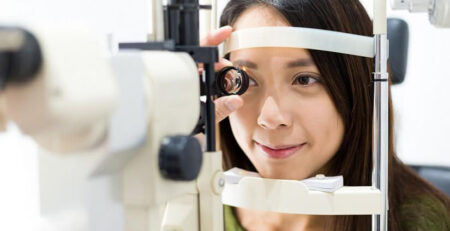
Therefore, managing blood sugar, blood pressure, lifestyle, and consulting the best eye specialist in Delhi are essential to controlling diabetic retinopathy. Routine eye exams by an ophthalmologist are necessary for detecting diabetic retinopathy early on because early detection enables prompt treatment, which can prevent or reduce visual loss.
Treatments for Diabetic Retinopathy:
A good control of diabetes is of extreme importance for long term benefit of diabetic retinopathy treatment. Here are some diabetic retinopathy treatment options:
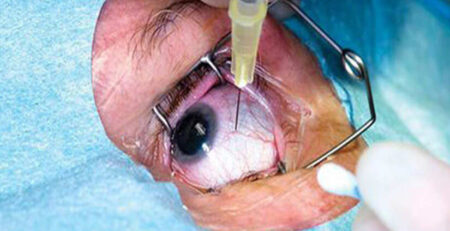
- Intravitreal injections are given monthly, depending on the severity of the swelling and blood sugar level.
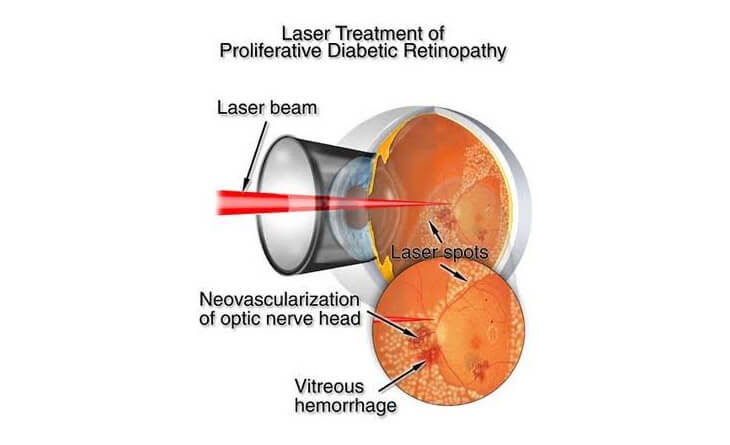
- PRP, or retinal laser surgery, is used to seal leaking blood vessels and prevent further damage to the retina. This treatment is often used for both non-proliferative and proliferative diabetic retinopathy.
Note: Depending upon the stage and macular condition, your doctor may prescribe either injections or lasers, or in some cases, injections and lasers are prescribed in combination.
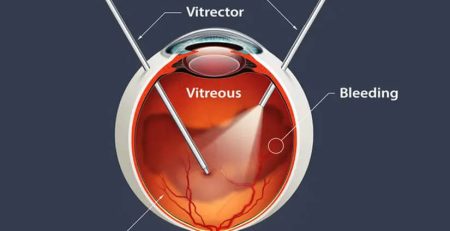
- Severe cases of diabetic retinopathy might require surgical interventions like vitrectomy, where the vitreous gel inside the eye is removed to address severe bleeding and scar tissue formation.
Final Words!
Diabetic retinopathy is a serious eye condition. Managing diabetes through proper blood sugar control, regular medical check-ups and a healthy lifestyle can be crucial in delaying the onset and progression of diabetic retinopathy.
If you are looking for diabetic retinopathy treatment, consult Dr. Anisha Gupta, a reputed eye specialist in Delhi with many successful eye treatments to her credit, and prevent further vision loss.